 (Photo credit: Wikipedia)
(Photo credit: Wikipedia)We’ve all been waiting for data to trickle out regarding actual outcomes from studies that have employed gait modification for the treatment of specific running injuries. Those data are now starting to appear.
A group led by Major Angela Diebal from Keller Army Community Hospital in West Point, NY just released a on-line version of a forthcoming 2012 article in the American Journal of Sports Medicine. The article is titled “Forefoot Running Improves Pain and Disability Associated With Chronic Exertional Compartment Syndrome.”
Chronic exertional compartment syndrome (CECS) is a condition that primarily affects active people (about 69% of those diagnosed are runners), and is characterized by swelling of affected tissues. There are four separate muscle compartments in the lower limb, of which the anterior compartment is most frequently affected in compartment syndrome. The connective tissues that encapsulate these muscle compartments do not stretch much, and thus excessive swelling in these compartments can lead to diminished blood flow to the affected tissues, as well as compression of nerves leading to pain.
Diebal et al. indicate that accepted belief as to the cause of compartment syndrome is “that exercise increases intramuscular pressure, which in turn compromises circulation, prohibits muscular function, and causes pain and disability in the lower leg.” They go on to state that “As the problematic exertional activity (typically running) continues, compartment pressures incrementally increase, which presumably causes increasing lower leg pain, sensory abnormalities, and muscle weakness, eventually resulting in a premature cessation of the activity.”
The Mayo Clinic website reports that “Conservative treatments typically don’t help with chronic exertional compartment syndrome. However, surgery is usually successful, allowing you — whether you’re a recreational or serious athlete — to return to your sport.” The surgery mentioned is known as a fasciotomy, and involves cutting the connective tissue sheaths surrounding the swollen compartment to reduce intracompartmental pressure (fair warning – if you have a strong stomach, you can see gruesome photos of this surgery here). Surgery can successfully treat the condition, but side effects are possible, recovery time can be extensive, and lets face it, if you can avoid having your leg sliced open that’s probably not a bad thing.
 Thus, the goal of this study was to determine whether an alteration in running gait could serve as an effective, and more conservative, alternative to surgery for the treatment of CECS. Previous research suggests that ankle position can influence intracompartmental pressure (ICP) in the anterior compartment (e.g., forefoot running decreases anterior compartment pressure, and ankle dorsiflexion increases ICP in the anterior compartment). Furthermore, the authors report that forefoot running has been shown to reduce eccentric activity in the tibialis anterior muscle (eccentric contraction is that which occurs while the muscle is lengthening, such as during the post heel-strike foot slap).
Thus, the goal of this study was to determine whether an alteration in running gait could serve as an effective, and more conservative, alternative to surgery for the treatment of CECS. Previous research suggests that ankle position can influence intracompartmental pressure (ICP) in the anterior compartment (e.g., forefoot running decreases anterior compartment pressure, and ankle dorsiflexion increases ICP in the anterior compartment). Furthermore, the authors report that forefoot running has been shown to reduce eccentric activity in the tibialis anterior muscle (eccentric contraction is that which occurs while the muscle is lengthening, such as during the post heel-strike foot slap).
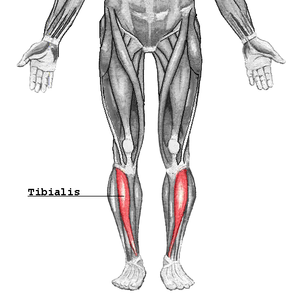
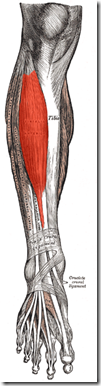
The tibialis anterior, shown in red in the image to the left (image via Gray’s Anatomy and Wikipedia), is the major dorsiflexor of the ankle and is found on the front, outer portion of your shin (it is the largest muscle of the anterior compartment; other muscles in the compartment include those that extend your toes upward). The idea is that by having patients with CECS adopt a forefoot striking running style, they would reduce pressure in the anterior compartment where this muscle is located, reduce eccentric activity in this muscle, and thereby reduce pain and disability associated with the condition.
The researchers recruited ten patients with CECS who were candidates for surgical intervention (as determined by an orthopaedic surgeon) – all were physically fit members of the military, and all had experienced symptoms for at least six months. Furthermore, all were confirmed as heel strikers, and pain onset occurred with less than five minutes of running.
After taking a battery of pre-intervention measurements {e.g., ICP, ground reaction forces, step length and rate, 2-mile run time, run distance before severe pain onset (up to 5km) etc.}, the subjects went through a training program to instruct them to forefoot strike with an increased cadence (3 steps per second, 180 steps/min). They also performed a variety of drills taught by the POSE method of running, and did some barefoot running and were cued to “run quietly.” Training sessions occurred 3 times per week for 6 weeks (45 minutes each session).
After the six week training period, the subjects went through a repeat battery of tests to determine the effect of the change in running gait. More interestingly, the researchers also did a minimum one-year follow-up with each patient to determine if the intervention had lasting success. Here’s what they found:
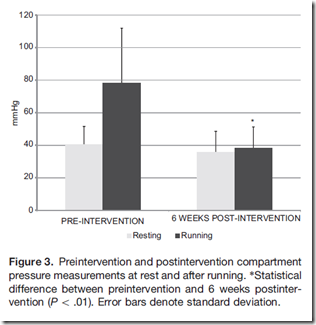
1. Intracompartmenal pressure (ICP) increased significantly from resting levels after a running bout prior to the intervention. After the gait retraining, ICP did not increase from resting after a running bout (see graph below from Diebal et al., 2012, American Journal of Sports Medicine).
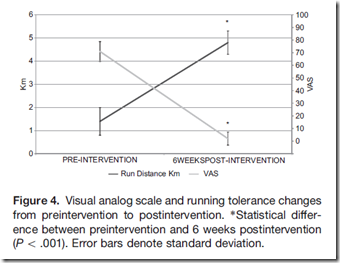
2. Running distance prior to severe pain onset (up to 5km) increased significantly post-intervention, and pain reported on a visual analog scale while running decreased significantly post-intervention (see graph below from Diebal et al., 2012, American Journal of Sports Medicine):
3. Step length, contact time, peak vertical ground reaction force, impulse, and weight acceptance rate all decreased significantly post-intervention. Step rate increased significantly.
4. At the one-year follow-up, 8 of the 10 patients reported that they were running a minimum of 5 km two to three times per week. The two exceptions were due to a torn ACL suffered while playing soccer, and a sprained ankle – neither of these individuals reported running limitations prior to the subsequent injuries. Mean 2-mile run times were significantly faster at the one-year follow-up.
5. All patients reported that they were able to participate in sports without limitation following the intervention.
6. Perhaps most importantly, none of the patients required a fasciotomy.
The results of this study are striking in that they are so uniformly positive, which somewhat overcomes the limitation of a small sample size and lack of a control group. For a condition that typically requires surgical intervention, to have ten individuals who were candidates for surgical intervention avoid surgery and return to normal activity levels as a result of modifying their gait is a very encouraging result. In fact, all but one of the ten individuals were able to complete the entire 5km run test with virtually no pain after the six-week intervention period, and follow-up after a year indicated that any changes that occurred during the intervention were retained long-term. I’m always hesitant to call anything a “cure,” but it’s hard to argue with these results.
The strength of these results suggests that gait modification could become a first-line treatment in the management of anterior compartment syndrome, and suggests that surgery need not be the fate to which sufferers of this painful condition must succumb.
It is also encouraging that these patients appear not to have experienced negative outcomes from the gait modification – altering foot strike and other aspects of stride can have unintended consequences, and it’s important to keep this in mind when applying an intervention such as this. For example, another study that looked at the effects of forefoot striking (via POSE technique) found increased power absorption and eccentric work at the ankle in POSE runners, but that study stipulated that runners not let the heel touch the ground (almost all runners I have observed let the heel touch down after initial forefoot contact). Given the mix of methods employed in the current study (cadence training, POSE drills, barefoot running), it’s hard to know exactly what the resulting form changes looked like. Nonetheless, we don’t want to simply trade compartment syndrome for Achilles tendinopathy or a metatarsal stress fracture, and it is encouraging that this appears not to have happened.
One of the reasons why this study is so gratifying is that it shows that applying biomechanical knowledge of the running gait to a particular injury can lead to a promising new therapeutic intervention. We know that heel striking increases pressure in the anterior compartment and probably works the tibialis anterior harder relative to forefoot striking. Thus, it makes logical sense that avoiding a heel strike might reduce symptoms associated with CECS and possibly “cure” the condition – it would appear that this is exactly what happened. What we don’t know for certain is whether a similar intervention might work for other conditions where the link between biomechanics and pathology is less clear. We also don’t know for certain which aspect of the running form change is responsible for these positive outcomes – was it the forefoot strike, or perhaps the reduced stride length or increased cadence that had the biggest effect. Hopefully future studies will attempt to tease this apart.
To end, I’ll note that a few months ago I listened to a British Journal of Sports Medicine podcast interview with Dr. Andrew Franklyn-Miller – he also reports success of gait retraining for the treatment of compartment syndrome, so we may really be onto something here…




















Hi Pete, this is a good study. My personal experience is very much along these lines. In my habitual heel-striking days my TA was way tight and always so enlarged that you had to work hard to get the fingers hooked onto the shin bone. After transition this area is much reduced in tension and size. Brian
Although it is not mentioned in the study. It was done using the Pose Method
It was mentioned in the study, and here in this post. They used Pose as well as cadence training and barefoot running, so a mix of techniques.
Sorry. I didn’t read the post carefully enough. My mistake.
Do they mention anything about Achilles or lower calf pains? That’s what I face nowadays as I transition. Quite annoying that.
No, the study was specifically looking at treatment of anterior compartment syndrome. Be careful with the Achlles, don’t want a case of Achiles tendinopathy! I’d tell you to be careful about forcing a forefoot strike, and always make sure to let your heel touch down. Also, don’t be afraid to use a shoe with some lift from time to time.
I had a bit of Achilles pain when I first transitioned, and occasionally still get a tiny bit. The thing that seems to alleviate this is to soak my feet in cold water after a run. Doesn’t need to be icy – in fact, if it’s too cold, that seems to lessen the effectiveness. Finally, focus on relaxing your feet and legs as you run. I believe attempting to change your gate can cause you to carry tension in your feet and lower legs, which interferes with proper function and recovery.
The treadmill really did a number on the calf, it always hurt after that. I found that if I did POSE which forces the foot to come back straight down, it didn’t hurt as much. But when I get tired and lose form something happens and I start to get calf pains. Will take your advice and go back to the Frees for a bit.
Hi Bwan
No one in the study experienced any calf or Achilles issues.
Angie
Great article, Pete!
I have had CS for years and in the last year have found that trying to adopt a more midfoot strike has helped slightly, more in terms of recovering to be able to run the following day.
But not to the point I can ever road race at race pace especially over shorter distances up to 10K.
I tend to stick to grass/trail which helps but am moving to NYC soon and am worried about the lack of proper trails close to me.
Am going for a pressure test on Monday as I am fed up with not being able to road race especially when I come to NY.
Does anyone have any recommended surgeon in the NYC area experienced in CS for possible future purposes?
Excellent post Pete. The study mentions that they were instructed to run barefoot a few times per week. Do you know if they made any other modifications? It would be interested to see if any of the study participants started in a stability shoe or orthotic and were able to move away from it.
Actually there were several participants who moved from using orthotics/stability shoes in the follow on study (see March 17 AJSM pre-view). I would be happy to answer any questions you may have on the study.
“”””We also don’t know for certain which aspect of the running form change is responsible for these positive outcomes – was it the forefoot strike, or perhaps the reduced stride length or increased cadence that had the biggest effect.”””””
It was probably all three that made the difference.
Hi Jeremy
Actually when you transition to a forefoot running style the decrease in stride length and increase in cadence follows suit. :). Several studies have been published demonstrating this concept.
Angie,
Thanks for your willingness to answer questions here. I would say that in most cases I would agree that forefoot striking typically occurs in conjunction with a shorter, quicker stride, but there are cases where forefoot strikers do overstride. Lieberman discusses this a bit in his recent paper in ESSR. It has also been observed that forefoot strikers who do not allow the heel to touch down tend to exhibit increased stiffness and increased tibial acceleration. So it can get a bit complicated when these exceptions to the general pattern are considered.
That being said, it makes complete sense to me that a forefoot strike would benefit someone with anterior compartment syndrome given what we know about the mechanics of the various foot strikes. It’s nice to see studies like this that actually employ form change as a tool for injury treatment and actually track outcomes.
Pete
Sent from my iPad
Thank you Pete!! And you are correct there are exceptions to every rule :) I’m appreciative that you chose my article to write about on your website :)
Angie
I was recommended for the surgery last spring, but wanted to try conservative methods first. I saw 1 primary care physician, 1 orthopedic surgeon, 2 physical therapists, 1 massage therapist, 1 chiropractor, 1 neurologist, and 3 personal trainers about it. Nothing worked. And no one suggested I learn forefoot running. This is the first promising research that offers an alternative to surgery.
I’m really excited!
If you simply think about the mechanics, it makes sense that this would have promise as a treatment. If you try it, definitely give an update!
Does it still make sense to try gait modification if you get the same symptoms from exercises that involve the leg muscles, such as mountain climbers or jumping lunges?
Do you have anterior compartment syndrome that manifests primarily from running? Or do you only get it when doing these other exercises?
—-
Pete Larson’s Web Links:
-My book: Tread Lightly: link to ow.ly
-Blog: https://runblogger.com
-Twitter: link to twitter.com
-Facebook Page: link to facebook.com…
-Discussion Forum: https://runblogger.com/forum
Hi, Pete, thanks for replying. I used to get CECS symptoms only from running, but since then I’d been wrongly diagnosed with shin splints and consequently went through a series of calf/shin/thigh/hamstring strengthening exercises which had eventually only exacerbated the condition. So now I get the same symptoms from running, hillwalking, racewalking, and leg muscle exercises, in the respective muscle groups: numbness, pain, difficulty moving the foot, etc.
Is it primarily on the outside front of the shin that you get symptoms?
When running on a flat terrain or racewalking, yes. The muscles affected are anterior tibialis, peroneus longus and brevis, and soleus. When running uphill or hillwalking: gastrocnemius. When doing wall-sits or lunges: quadriceps. When doing squats: hamstrings.
Sounds like you are prone to this in multiple muscle compartments. Would be interesting to take a look at your stride – gait change to a forefoot strike might help the anterior tib/peroneals, but could exacerbate the soleus since it takes on the brunt of the work in a forefoot strike. The article linked is aimed at treating people with isolated anterior compartment syndrome and apparently no issues in other areas. wish I could be more helpful!
—-
Pete Larson’s Web Links:
-My book: Tread Lightly: link to ow.ly
-Blog: https://runblogger.com
-Twitter: link to twitter.com
-Facebook Page: link to facebook.com…
-Discussion Forum: https://runblogger.com/forum
This is a pretty cool stuff. It is a real shame that there was no control. I’d be curious, Pete, as to what you think the proper control group would be for this study.
Control group would have to be individuals with CECS with whom you did not impose the study variable, in this case, gait retraining. So in other words, expand the study size. Randomize patients to control group vs. gait retraining. After your period of prescribed intervention, compare the gait training group to those that you did not gait train. Seems like this might be the next logical step to bolster the validity of this study.
Or have the control group come and run three times per week as the study group did, but provide no instruction or advice and have them stop the moment pain appears.
…and hope the ethics committee turns a blind eye…
Yes, probably why there was no control group :)
We are actually in the process of conducting an RCT at the moment Josh :). More to follow!! :)
A diagnosis of CECS in the anterior compartment was exactly what motivated me to begin addressing my running style (stride length and cadence, foot strike, posture, and shoes). You mention the strong stomach needed to look at the images from the surgery, but the ICP diagnostic test itself, as described by my ortho and by YouTube videos, was too terrifying to submit to. A friend recommended Born To Run, and I was back to running 10+ miles within a few months (I was limited to about 2 with CECS symptoms).
I certainly wouldn’t wish CECS on anyone, but the sensation of losing feeling and circulation to the part of my foot that is controlled by those muscles in my anterior compartment actually helped train me to run more gently and land on my mid/forefoot. When I experienced pain, it was because I was trying to snap my toes back quickly enough for my heel to catch the impact of the footfall. When I responded naturally to the pain – running a little more mindfully – I found the best way to protect myself was to not try snapping my toes back, which meant landing further up my foot. The CECS was actually a good “coach” (as perverse as that sounds) for forcing my strides back to a reasonable length and moving my landing pad toward my toes. When I first heard the advice (on this great blog, no less) to try to “land with your foot behind you,” I realized that’s what I’d been less consciously working toward.
All that to say CECS sucks hard, but it got me to a much better place as a runner. I’ve lost more weight and set more PRs in the ~24 months since then than I did in the previous 5 years.
Thanks for sharing – this is the kind of story that keeps me motivated to continue blogging!
Just like week I had a bout of sore/tightness/inflammation of my left tibialis anterior. The cause looked to be a heel striking descending steep and prolonged descent. I was wearing my Roclite 295’s that have a 9mm heel drop which make it awkward to land on my mid-foot when descending. These days I don’t heel strike too much so my shin muscles won’t be getting the work out to strengthen enough to handle to quick steep descents.
The solution for me was to get back into my zero drop Neo Trail’s to make sure I wasn’t heel striking, and to message the belly of the muscle. The message made it rather tender initially but then it just cleared up after a couple of days.
This afternoon I completed a 27 mile training run in Roclite’s, the route included some gentle descents and had no problems with my shins at all. This is one week after aggravating my shins, to an extent that I feared I might have a difficult to shake injury, but as it turned out getting off my heels and back exclusively onto my mid-foot and a short bout of specific message did the trick.
For me there isn’t any doubt that heel striking will be the predominant cause of shin injuries. It’s my own personal experience, and it fits from the perspective of how that muscles are used in different gaits. When landing mid-foot or on the forefoot simply doesn’t eccentric loads the shin muscles. Not only will heel strike cause an eccentric load on the shin muscles on landing, the higher the heel and the higher the relative speed on contact the higher the moment on the ankle and higher the eccentric loads need to be avoid heavy foot slap.
I would expect that running with a higher cadence and with less over-stridding and lower heels one would be able to reduce the eccentric loading of the shins even when heel striking. However, with heel striking you’ll never be able to eliminate the eccentric loads on the shin muscles completely.
However, if one lands mid-foot or on the fore-foot one will be able to largely eliminate the eccentric loads on the shin muscles. It won’t matter what the cadence is, what the rest of your running for is like, if you don’t land on your heel you won’t be eccentric loading the shin muscles so should be able cure it without any other adaptations required.
Given the last two observations it’s a shame that this research didn’t just isolate what is likely to be the key factor in success. Instead the chose to adopt “Pose Method” and other factors which rather clouds the key factor. Doing similar study using just the foot strike adaptation would be useful.
Studying other interventions like using lower heeled shoes, increasing cadence, message therapy etc would all be useful. However, looking at what causes eccentric loading of the shin muscle I would suggest that it’s the foot strike that will be single most important factor to adjust.
One but is… changing foot strike isn’t easy, and it isn’t risk free, so perhaps the other interventions could used well. However if a running is chronically injured already and unable to run then doing a complete reset and starting from scratch with changing foot strike and slowly building up might be safe. If one just has niggling problems with shin problems then perhaps just changing cadence or footwear might be sufficient to keep the problem under control.
Great points Robert – I agree with your suspicion that the forefoot strike alone may be enough to offload the shins, but also agree that it’s probably safer to transition to a forefoot strike in association with a shortening of stride and increased cadence.
Sent from my iPad
I had a patient come in after having this surgery, with a ton of complications post-surgery. Too bad she wasn’t told to explore running efficiently on the forefoot, before doing an intervention that was so invasive.
Is chronic exertional compartment syndrome (CECS) a more specific term for the generic condition generally referred to as “shin splints”?
Not the same thing, but shin splints is sometimes used as a catchall term for any kind of shin pain. Compartment syndrome is due to increased pressure in the muscular compartment, whereas shin splints are typically pain at the insertion of the muscle on the tibia due to excessive pulling of the muscle on the bone.
I think the next natural question is…
“Is forefoot/mid-foot running a cure for most types of shin injuries?”
My guess is that answer is probably yes. It won’t be the only cure, but certainly “a cure” for a lot of cases.
This study obviously doesn’t address general shin injuries, or the foot strike specifically, so extrapolating right now is just an educated guess given the mechanics of heel striking vs non heel striking. However, a study configured to test this hypothesis would be a useful step.
I dealt with compartment syndrome for a couple years. Finally started to come out of it mid last year without any conscious change in terms of stretching or foot strike. Allowed me to ramp up my miles increasingly throughout 2011. Prior to that, there were times I might only be able to run 0.5 mile before hobbling home.
Started to get a re-occurrence late last year, but began aggressively stretching my calves using a belt. Even though the pain was on the shin, calf stretching seemed to help. Having started to switch to a mid/fore foot strike which seems to help as well which also requires calf stretching.
Be able to run about 10 miles per week for several months since without pain. Before I got it under control, I could only manage about 3-5 MPW and they were painful. Don’t care what fixed it, just relieved to be able to run pain free.
It’s a sample size of one, but I had been suffering from horrible CACS when I started seriously running again. Calf sleeves worked for a while, but after a time even that stopped helping. I knew what the surgery entailed so I avoided it as long as I could, but I knew it was a matter of time.
Then I started forefoot striking, (for other reasons), and the pain literally disappeared overnight. It was gone totally (along with the near-crippling posterior shin splints). So I am convinced that there is something to this.
Careful with the sleeves (they are intended to increase pressure)
Pretty terrible study scientifically and extremely ambitious conclusion based on the lack of controls. I’d hardly say that running 5k 3 times a week is a true cure either. I had been mis-diagnosed with a ruptured gastroc the last few years only to find out I have compartment syndrome (all 4 compartments now in both legs). The initial faciotomy (on my left) got me back up to 60 mpw before the right leg started to flare up, now I’ll gladly go under the knife again, with hopes that I’ll get back to my college mileage of 70-80 mpw.
BTW, I am and have always been a fore-foot striker
Echoing what many have already said, wish only one variable at a time would have been changed. That said, here is what I know in my own experience. Barefooot, Zero drop, or slight drop, a mid to forefoot strike seems to have definitely allowed more control over my CACS. It seems that there are several factors at play in my experience so far: dorsiflexion ( or perhaps excessive) seems to contribute – if I just sit down and do repeated dorsiflexion I can exacerbate the condition, tight calves – if I stretch them out a bit as I feel the onset it helps delay or eliminate, easing into a run so that the calves “warm up a bit”. I have been playing with massaging and ice after a run as well. The next step is resolving the increased Achilles and Calf pains – to much to soon, mechanics, etc.
Man! I wish I’d seen this 15 years ago. I’ve had CECS for 15 years (I call it shin lockage) and it’s really a mystery to me why I can run marathons, half marathons, 10k’s and 5k’s without getting it then I’ll get it for no apparent reason. I’ve been able to come to some conclusions, though: I don’t get shin lockage if I sprint or do hill repeats (running more on toes?). Also, if I weigh less I get it less. Working out the day before helps but don’t know why. There was a time where massage before running helped but that has become hit and miss. Putting a heel wedge has helped but also hit and miss. What I hadn’t tried is barefoot/minimalist/toe running. I will try it tomorrow!
Sprinting + running up hills = more forefoot gait. Right in line with what this study showed :)
—-
Pete Larson’s Web Links:
My book: Tread Lightly – link to ow.ly
Blog: https://runblogger.com
Twitter: link to twitter.com
Facebook: link to facebook.com…
Any luck with the form change and your CECS?
—-
Pete Larson’s Web Links:
-My book: Tread Lightly: link to ow.ly
-Blog: https://runblogger.com
-Twitter: link to twitter.com
-Facebook Page: link to facebook.com…
-Discussion Forum: https://runblogger.com/forum
I haven’t had a chance to experiment due to tearing some ligaments in my knee. Hopefully I’ll get cleared to run by next month.
Sorry to hear about the knee!
—-
Pete Larson’s Web Links:
-My book: Tread Lightly: link to ow.ly
-Blog: https://runblogger.com
-Twitter: link to twitter.com
-Facebook Page: link to facebook.com…
-Discussion Forum: https://runblogger.com/forum
I’m back to slow running but get “shin lockage.” The reason is that I’m favoring my injured leg and land heavy on my CECS leg. This should get better as my injured leg gets stronger and can even out my stride.
I bought the Altra shoes but they don’t work in preventing CECS for me. Today, I went back to putting wedges in the heel part of my shoes. I was able to run further since my knee surgery without getting the shin lockage. The wedge forces me to land more on my toes when running so still convinced forefoot running works with this condition.
I have film of people continuing to heel strike in Altras, I really think conscious alteration of form may be necessary unless you go to a very minimal shoe, which carries other risks. In this case the forefoot landing is what will take the load off of the anterior compartment.
Sent from my iPad
Calves are sore from running with heel wedges in my shoes. Kinda like running with high heels but no shin lockage! I wish they made shoes with built in heel wedges but not how theyake them now…cluncky and heavy heels.
This is encouraging but a few things don’t add up for me. As a former sprinter, I have always been a forefoot striker yet I appear to have suffered through decades of misdiagnoses (typically shin splints) before I was tested recently. My pre-exercise resting pressures were Right: 29mm Hg and Left: 46 mm Hg in the anterior compartment. The other compartments were as high or higher and the differences were correlated with existing herniations of the fascia. Post 5 minutes of walking on a 10% slope, I was over 110 mm Hg. I even get it wen out of the saddle on a road bike. I’ll be sure to return to a forefoot strike after I’ve recovered from the bilateral, 4 compartment fasciotomies. I’d be interested in hearing anyone’s experience with recovery. At day 6 my left leg is doing well but my right leg is still swollen.
THANK YOU THANK YOU. I was diagnosed with ECS about two years ago. My doctor told me to try physical therapy for 8 weeks and if that did not work that maybe I needed surgery. I knew that I did NOT want surgery. I tried PT for 8 weeks and it didn’t work. I experience the effects of ECS about a half mile in. I get the visible swelling in my shin, tightness, muscle weakness. I walk it off for a bit, run again, get the pain again…walk it off….this walk/run lasts for about 3 miles until the ECS symptoms disappear for the remainder of my run. I have no idea why this happens but I am glad it does. The fact that it does disappear caused me to never use surgery as a option. This past weekend, I ran my 7th half marathon. Did the usual walk/run for first 3 miles until the pain/tightness/weakness left. I was a bit disappointed that I did not set a PR so I became focused on finding a way to beat this ECS without surgery. I am so glad I stumbled upon this blog. I found some videos on YouTube about front foot running. I will try this tomorrow. Wish me luck!
My best advice is don’t try too hard to force a forefoot strike or you may precipitate problems with the posterior compartment. The idea is to make contact along the pad behind the little toe, then allow the heel to settle to the ground. You might also try a flat shoe as it will make the process much easier – something like the Altra Intuition or Skechers GoBionic or Merrell Bare Access.
—-
Pete Larson’s Web Links:
-My book: Tread Lightly: link to ow.ly
-Blog: https://runblogger.com
-Twitter: link to twitter.com
-Facebook Page: link to facebook.com…
-Discussion Forum: https://runblogger.com/forum
I ran 5 miles yesterday. No heel striking…no shin issues. Amazing. I can’t believe the “cure” is so easy. I can’t believe my physical therapist or orthopedic doctor never recommended this to me. It is taking some extra concentration to forefoot strike. I found myself falling back into heel strike a stride or two but I quickly corrected it. Practice makes perfect.
What would you suggest of someone with CECS in anterior compartments but also severe tightness in posterior compartments? It seems that switching to forefoot running style only transfers the forces to the back of your calves as it relieves the pressure from the Tibialis anterior.
Tough call. In that case I’d really focus on midfoot strike and relaxing the lower leg below the knee. Imagine the ankle dangling loosely from the leg, avoid tensing either front or back prior to contact.
Great article! I run high school cross country and have had to take the past 2 months off due to CECS. I have been to physical therapy and saw no improvemts. I want more than anything to start running again with the team. Is it normal to feel pain at rest? Also, is it harmful to just run through the pain?
Which part of your leg is giving you the trouble? Problem with CECS is if your form is causing the muscles to work in such a way that the compartment continues to swell it’s unlikely to resolve if you just run through it. Did the PT video your running form?
It is the upper muscle right next to the shin bone on the outisde, along with tight calves. They did videotape me and I am a slight overpronator.
In the spot indicated by the arrow here: link to painfreefeet.ca ?
What shoes do you run in?
Yes that is exactly the region. I run in Asics GT-2000 but used to run in Asics Gel Nimbus.
Is the compartment syndrome only on the front of the shin? If you just have tight calves and not compartment syndrome in the back as well then moving to a shoe with a lower heel and working on form (moerating heel strike if you tend to do that) might be a worthwhile approach, maybe in association with some foam rolling of the calves. Definitely something to do under guidance of your PT though in case problems crop op – there can be some transition risk with form change.
Is the compartment syndrome only on the front of the shin? If you just have tight calves and not compartment syndrome in the back as well then moving to a shoe with a lower heel and working on form (moderating heel strike if you tend to do that) might be a worthwhile approach, maybe in association with some foam rolling of the calves. Definitely something to do under guidance of your PT though in case problems crop op – there can be some transition risk with form change.
I am experiencing pain in the calf region.
Will Newton brand shoes help?
Depends on what you are running in now and what the specific problem is. Newtons tend to be lower drop than most shoes and this can actually put more stress on the calf.
I know this is an older article, but I had to comment. I just returned from a pressure test for anterior CECS with a surgery date six weeks from now. I was actually looking for success stories online, but when I saw this title I was so curious. I’ve been dealing with this for 6 months — all road running. Two days ago, weather and timing didn’t allow for it so I ran on the treadmill (gasp) waiting to feel the familiar burning and tightening that I feel on the road after about 10-15 minutes. When 20 minutes passed and I was still running fine, I upped my pace. Thirty minutes passed, nada. At 40 minutes i increased the incline and waited. By 55 minutes with no sign of the pain, even though I adjust my gait to try to bring it on, I could not recreate the pain. I mentioned this to the doctor performing my test today and he said yes, on the treadmill you have less need to heel strike. Yet when my road run produced high pressure readings (even my resting was high) he never mentioned trying to change my gait. He mentioned changing sports and when I grimaced he launched into possible complications with surgery, then we set up the surgical appointments. I meet with my primary sports doc soon to go over the results and I am absolutely going to look more closely at gait studies to see what we can come up with in the next 6 weeks. I’m absolutely heartened at the idea of a surgery-free recovery. Thanks for sharing this and now I’m off to delve more closely into this possibility. (and sign up to follow your blog.) Best, Tara
Tara – is your issue in just the anterior compartment? If so, may really be worth considering trying gait change and maybe a zero drop shoe to see if it might resolve the problem and help you avoid surgery. What part of the country do you live in? There are folks around who specialize in gait retraining and I might be able to provide a suggestion.
Since there are a few comments still, here’s my experience:
I had anterior CS in high school and extremely tight calves. Everywhere in my lower leg was tender and tight. My shin muscles were pretty jacked and my calves nonexistent. This was early 2000s, so no one recommended these particular gait changes. I had surgery but ultimately stopped running. I regret the surgery. I still have CS symptoms.
I have a twin sister who never had CS. She has a naturally bounding gait and definitely tends toward more mid or forefoot landing. I was a heavy heel striker. With pain I did slow down and land more on the midfoot, but by then the pain was pretty set in.
About a year prior to the CECS, I had major abdominal surgery and my body alignment completely changed. I began curling my pelvis forward against the painful scar tissue. This locked up my hips and butt, and tightened all down the outside of my legs. No wonder I was such a heel striker.
I’d like to run again but my body is so locked up I need some huge PT but don’t know where to start.