 If you wear running shoes, it’s fairly likely that you are familiar with the so-called “wet-test.” The basic procedure is that if you wet the sole of your bare foot and stand on an absorbent surface like dry concrete or a paper bag, the imprint of your foot will reveal something about your arch height (my wet-test result from last summer is shown in the image to the left).
If you wear running shoes, it’s fairly likely that you are familiar with the so-called “wet-test.” The basic procedure is that if you wet the sole of your bare foot and stand on an absorbent surface like dry concrete or a paper bag, the imprint of your foot will reveal something about your arch height (my wet-test result from last summer is shown in the image to the left).
Typically, the results of the wet test are interpreted as follows. If no distinct arch is visible, you have flat feet, probably overpronate, and thus need motion control. If there is a distinct dry area under the inner side of the arch region of your foot with a complete wet band adjacent to it on the outer side, you have normal arches, normal pronation, and would do fine with a mild stability or perhaps a neutral shoe. If the outer wet band is separated in the middle by a dry area, or if the wet band is very narrow, you have high arches, underpronate, and need a neutral cushioned shoe. This 2004 article from Runner’s World website provides a typical example (with diagrams) of how to interpret your “wet test” results.
Unfortunately, there’s a big, big problem with the wet test, and it’s due to the fact that the test is done when you are standing still. This is what’s known as a static measure of arch height/deformation/collapse, meaning we take it while we are not moving. Though we all might feel like we are standing still sometimes when we run, I can assure you that running involves movement of your legs and feet, and we don’t need a scientific study to prove that! When we run, forces generated are very different than when standing still, and the arch of the foot behaves differently. Why? Because the arch is not simply a passive structure. There are muscles that help to support the arch, such as the tibialis posterior and the flexor hallucis brevis, and it’s quite likely that they are going to be more active when you are running than when you are standing still.
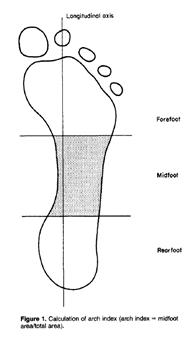 Several scientific studies have shown that static measures of arch height yield significantly different results than those measured while walking or running (dynamic activities). In a study published in Clinical Biomechanics in 1989, Dr. Joseph Hamill and colleagues from the University of Massachusetts compared static and dynamic (walking) footprints using a measure called arch index. To determine arch index, they applied ink to the feet of their subjects, had them walk over sheets of paper, and compared the size of the ink imprint in the region of the midfoot relative to the overall area of the foot imprint (excluding the toes – the shaded region in the picture at left shows the midfoot area compared by Hamill et al., 1989).
Several scientific studies have shown that static measures of arch height yield significantly different results than those measured while walking or running (dynamic activities). In a study published in Clinical Biomechanics in 1989, Dr. Joseph Hamill and colleagues from the University of Massachusetts compared static and dynamic (walking) footprints using a measure called arch index. To determine arch index, they applied ink to the feet of their subjects, had them walk over sheets of paper, and compared the size of the ink imprint in the region of the midfoot relative to the overall area of the foot imprint (excluding the toes – the shaded region in the picture at left shows the midfoot area compared by Hamill et al., 1989).
Hamill and colleagues found that arch index (size of the shaded area) increased in seven subjects, decreased in 15 subjects, and did not change in two when they compared the walking footprints to the standing footprints. Though static and dynamic measures were strongly correlated in this case, they were found to be significantly different, with the arch tending to be higher when walking than when standing. They suggest that differing orientations of the lower leg, increased weight bearing, or increased activity of foot musculature could explain the differences observed. They also found little correlation between observed arch index and other dynamic aspects of gait, writing that “the lack of significant findings between the dynamic aspects of gait and arch index may discount the use of this measure in functional lower extremity evaluation.” Furthermore, they write that “Although a large contact area may be present, very little force may be exerted over much of the contact area. A person who has a very large arch index may actually demonstrate a pressure distribution pattern more closely resembling a person with a very high arched foot (small arch index).” Finally, the authors do indicate that “first ray mobility was particularly effective in predicting dynamic function, supporting its continued use as a measurement in lower extremity evaluation.” So, the take home message seems to be that footprint type isn’t all that useful when it comes to predicting walking gait, but mobility of the first metatarsal and big toe are very important.
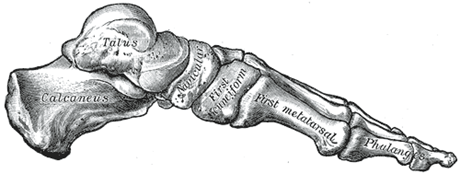
Jay Dicharry and colleagues from the University of Virginia published a paper in 2009 in the Journal of Orthopaedic and Sports Physical Therapy in which they did a bit more elaborate assessment of static arch deformation vs. dynamic arch deformation during walking and running. They did this by comparing values obtained from a static functional navicular drop test (see image below for navicular location), a static subtalar navicular drop test, and measures obtained by 3-D video analysis of arch height during gait (using markers placed on the foot).
Bony structure of the medial longitudinal arch of the foot – navicular bone is located near the apex of the arch – Photo from Gray’s Anatomy via Wikipedia
The functional navicular drop test sounds complex, but in reality is quite simple. The navicular is a bone in the midfoot near the apex of the medial arch, and the functional navicular drop test compares the height of the navicular during relaxed seated (non-weight bearing) vs. relaxed standing (weight bearing) positions. Higher values for functional navicular drop would thus indicate a greater degree of arch deformation/collapse, and thus a floppier, more mobile foot. Lower values for functional navicular drop indicate a more rigid arch that does not compress much. The second static test – the static subtalar navicular drop test – compares navicular height when the foot is placed in “neutral” position to when the foot is allowed to relax and compress the arch.
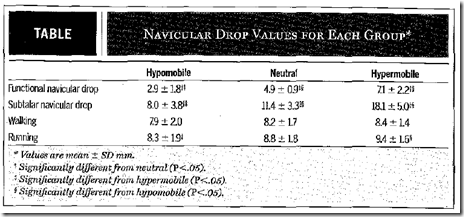
Results of Dicharry’s study (see below) showed that despite significant differences in arch collapse between the groups during static testing, arch collapse was identical in all three groups during walking, and the only difference observed during running was a small but significant difference between the hypermobile and hypomobile groups, neither of which were significantly different from people categorized as neutral (i.e., only the extremes were different, and the magnitude of the difference was far smaller than would be found using the static measures). Furthermore, despite increase in force magnitude during running, only the hypermobile group exhibited greater arch compression during running as compared to walking. They suggest that neuromuscular control during dynamic movement could explain these differences – basically, the brain activates appropriate musculature in the foot and legs to manage the forces and maintain the arch during walking and running, and this is not captured by measuring the arch when we stand still. The basic message is that even if you have flat feet and your arches collapse when you stand still, your arch may behave very much like the foot of a normal arched person when you are walking or running, likely due to muscular control.
This brings us to paper number three, which was just published on-line in Gait & Posture. The authors, led by Jesper Bencke from Copenhagen University Hospital in Denmark, compared measures of static navicular drop to both 2-D and 3-D measures of arch deformation during walking. They found only a moderate correlation between static measures of the arch and those obtained during walking (r2 = 0.31 for you stats oriented folks), and conclude the following:
“Assuming the foot as a two-segment structure in the sagittal plane with a hinge joint placed at the navicular bone between the forefoot and the hindfoot, the increased plantarflexor moment during push-off would correlate to an external moment attempting to dorsiflex the forefoot with respect to the hindfoot. The lack of good correlation between static and dynamic measures could thus be a result of this extra load being counteracted differently between participants. This would further imply that a static test measuring the ND (navicular drop) might only have limited validity as predictor of MLAD (medial longitudinal arch deformation) during gait.”
And these are not the only three papers that have shown this – if you’d like to read the full text of one you can take a look at Deng et al., 2010, who found no relationship between navicular drop measurements and arch deformation measured during walking.
So what does all of this mean? Basically, it tells us that what the arch looks like and how it deforms when we are standing or sitting probably doesn’t tell us much about what the arch does when we are actually moving. Thus, applying the “wet footprint” test as a basis for determining foot type, and thus as a basis for choosing a running shoe makes very little sense. If you are in a shoe store and they suggest that you try this test or if they take a look at your arch while you are stationary, be very wary of any advice that you get (this probably applies to those fancy foot scanning machines as well). As Dicharry showed, only the extreme floppy and rigid feet differed in degree of arch deformation during running, and the difference was very small and of unknown clinical significance (and neither differed from so-called “neutral” feet). What’s more, we have several studies showing that assigning shoes based upon arch height provides no benefit in terms of injury outcomes when compared to simply assigning everybody a stability shoe regardless of foot type (see here and here for examples).
All of this does not mean that some individuals with extremely rigid or mobile feet might not benefit from some tailored shoe advice, as studies do suggest that individuals with extremely flat or rigid arches do seem to suffer different types of injuries. However, it does suggest that the wet-footprint test as a general tool for assigning shoes should be put to rest. At the very least, methods that provide clinically relevant measures of arch deformation dynamically and simply and without a requirement for expensive gait analysis equipment that is rarely found in a shoe store should be investigated (e.g., the 2-D method described by Bencke et al.).

















G’day Pete, A fantastic article. I wonder how long it will be before shoe companies adjust their sales and marketing materials to recommend fitting shoes to the way you run rather than basing the decision on the shape of your foot?
Thanks Brian!
Sent from my iPad
there was a nice talk at the IRRA conference (http://www.therunningevent.com… in austin this week by the gait guys on their new 3 part fitting process they are rolling out in january. intended audience is running speciality retailers and medical folks, i believe.
it takes into account some static factors (forefoot/rearfoot varus/valgus, forefoot flexibility, etc), but more dynamic stuff too. we only saw an intro.
i took video from the entire 2 hour talk but only have a couple 14-15 min clips uploaded so far. will try to get the rest up soon – feel free to share, pete. link to youtube.com…
Interesting point – we tend to think of the foot length in isolation, neglecting potential variation in the relative lengths of the arch, toes, etc. Just looking at pictures of feet it’s clear that toe length is quite variable!
The main focus of shoe companies (as with all companies) is to make money and get people to buy shoes as quickly as possible. Here in Australia the biggest chain of sport shoe stores has a pressure pad thing you stand on which shows an image on a screen (bascially a glorified wet test) and they use this as a basis for recommending shoes. I was once talking to a guy that worked there and I asked hm why they don’t have a treadmill and he basically said that it takes too long and 95% of people who buy running shoes don’t really run in them anyway so it doesn’t matter if they are not the perfect shoes. They just want to get people in and out as quickly as possible and most people believe the pressure pad thing is scientific anyway.
We have a local store that has one of those pressure devices – common here in the US as well. The customer is supposed to be wowed by the technology, and the computer tells them what shoe they should wear. How can a computer be wrong! (sarcasm intended)
Um. Yeah, I’ve done the wet test running. but you’re right. Articles by slow bloggers who study animals (and make $$ off the craze), slow-mo vids of elites and books filled anecdotes about how barefoot running saved some douche is the way to go.
Wait, humans aren’t animals??? Oh, and I’m quite happy being a slow blogger :)
Sent from my iPad
You’re an animal Pete, I am way slower than you! Great article. I totally chose the wrong profession as I spend all day avoiding my real job and reading the stuff you do!
Ha! Thankfully I’ve managed to shift my day job focus so that it more closely meets my interests :)
Any other hobbies besides trolling?
I had a hunch! The first time I went into a running specialty shop was about 8 years ago, and I didn’t want to do the wet test or have my feet touched and measured, just because it seemed like a waste of time. I just asked to try on several pairs of shoes and jog down the strip mall in them. The sales people looked so uncomfortable! But, I got two pair of shoes that I wore, and wore out!
Also, I have been reading your posts for about 6 months now, I think and I want to thank you for sharing citations and not dumbing things down (for lack of a better phrase) You really know your audience and it’s great!
And, (sorry) I have a question, I have been working on my gait for about 18mos and have made significant progress, injuries are at bay, and I feel great (and faster). I have been wearing kinvara’s (but now the toe box is to snug) and rotating a couple pair of neutural mizuno’s. I took a pair of NB minimus road shoes for a test run (only a mile) a few weeks ago and my stride and feet felt really relaxed so I want to go purchase them. However, are you still supposed to buy a size up as with a typically running shoe? I know they are designed to go sock-less, which made me think they are to be more snug? (fyi, my day to day and dress shoes are 8’s, running shoes 9’s).
Thanks!
hi annabelle,
i’m a running retailer and a big fan of pete/blaise/etc. i agree a lot with what they say. for shoe fit, it’s important to have the running store employee measure both your foot length (at the toes) AND your arch length (while standing of course). they should use a brannock device, the heavy metal thing you’ve seen at shoe stores all your life.
if your arch length is much shorter or longer than average for your total foot length, the toe joints may not line up in the shoe where it’s designed to bend. this can put extra pressure on your feet in a bad way, especially if you are wearing more of a traditional shoe with more cushioning and less flexibility.
most people know to have space between their toes and the end of the shoe, but the arch length thing is not as commonly mentioned.
Superbe post Pete, For me there is 2 problems : #1 find something wrongHealth professionals (all professions included) and biomechanicians look in their patients the pathologies described in their medicine textbook. And when we search… we find. So they always find something to correct, something they consider not normal when normal itself is not defined. But is absolutely not clear if those peculiarities are really the cause of some pathologies. What to think about non-standard anatomical and biomechanical features like the right foot pronation of Haile Gebrselassie, the right knee dynamic valgus vector and right foot external rotation of Geoffrey Mutai, the anterior pelvic tilt of Buzunesh Deba… bigger than all our patients…#2 fix it with the wrong toolExactly like you said in your post… Your 2004 Runner’s world article is every year repeated by other magazines, shoe shop publicities and companies (like the ASICS Spring 2011 reference guide).
Blaise
I agree that we should emphasize that normal biomechanical (anatomically constrained) variation is just that – normal. I would say that is it is clinically important to remember that running and/or activity is for all people – many of whom are not athletes. It is wonderful that some of the world’s best runners are illustrations of curious biomechanics such as G. Mutai and H. Geb – they are well adapted to their unique biomechanical milieu.
Great article Pete!
it helps when you grow up barefoot and develop musculature to handle those styles! but agreed…there’s no one perfect form…just a perfect form for each of us.
Well put Eric, I agree.
Pete-Excellent post and perhaps one of my favorites you have ever done. After years in specialty running, you wouldn’t believe the fitting techniques I have seen. In a few of the studies it looks like arch index could decrease when walking. Do you know if it decreased even more when running? This is great news for us “static flat footers” who have been told we were broken. Thanks again Pete!
Thanks for posting this article, I’m glad dat it is now scientifically proven that I’m not some freak of nature ;-) If have genetically flat feet, was born with it, inherited those from my father. As a child I always felt the urge to run instead of walk form A to B. Then one day a doctor looked at my feet and decided that I defenitely needed orthotics. Even though I had no complants or what soever. These things were horrible, made my feet cramp and ruined my shoes inside. I didn’t wear them for long. As I started my LD running career years later, I was always advised stability or even motion control shoes because of the flatness of my feet. The weight of the shoes and the support elements always felt very uncomfortable. So I choose neutral shoes and transitioned to more and more light weight shoes over the years. Now I wear racing flats, the kinvara and hattori. I run a 50 k last saturday (not a competition but some sort of fun ultra event) on my flat feet in the hattori without any trouble. Okay, a little bit tired afterwards, but three days later fully recovered and up and running :-) Just another anecdote showing that the wet test is definitely not the right way to find the right shoe. For me and probably for a whole lot of other runners as well.
Thanks for sharing your experience! I think your story is quite common for people with flat feet, and it need not be that way.
Hey, Pete,
Thanks for posting a fabulous article. I just seems to validate the emphasis on minimalist or ≤4mm drop shoes as being the best way for the greatest number of runners’ feet to “do the right thing” by not being interfered with by over-designed, over-built, and over-priced shoes.
Static Analysis will NEVER be sufficient for determining proper footwear – and clearly not sufficient for determining which $500 orthotic one should be prescribed.
Active analysis is the only way to even begin to get at what is going on with a particular runner.
Thanks for the post Pete. I agree the wet-test can be very misleading. I suggest people look at their old shoes to see how they wear out. The wet test for instance says I have flat feet and so would need “stability” shoes..but my shoes wear out like those of an underpronator.