 A little over a week ago I published a post that addressed some potential causes of metatarsal stress fractures in new barefoot and minimalist runners. That post, by Dr. Casey Kerrigan, got quite a response, so I wanted to follow up with an additional post by a running radiologist by the name of Dr. Andrew Lischuk.
A little over a week ago I published a post that addressed some potential causes of metatarsal stress fractures in new barefoot and minimalist runners. That post, by Dr. Casey Kerrigan, got quite a response, so I wanted to follow up with an additional post by a running radiologist by the name of Dr. Andrew Lischuk.
Andrew currently holds the position of Assistant Professor in the field of musculoskeletal radiology at Yale-New Haven Hospital. He did his radiology residency training at Robert Wood Johnson University Hospital in New Jersey, and was fellowship trained in musculoskeletal radiology at Yale-New Haven hospital. He has been an attending radiologist for two years now. In addition to also being a doctor and runner, Andrew let me know that he’s most proud of being a devoted husband to his wife Kim, a dermatologist by trade who keeps him lathered up in sunscreen, and a dad to the best four year old on the planet, Reese!
I asked Andrew if he would share some thoughts on metatarsal stress fractures from the point of view of a radiologist, as he sees more than his fair share of fractures in his line of work. In particular, I asked him if he could address the topic of bone remodeling, or how bones react in response to stress. I hope you find what Andrew has to say both interesting and informative!
Metatarsal Stress Fractures: Thoughts From a Radiologist
For the past thirty years the incidence of metatarsal stress fractures has remained at or about 16% of all stress fractures ( Queen et.al. 2009). Numerous studies have been done over the last few decades looking at the factors involved in the development of stress fractures and how we approach them. In the process of replying to several of the responses I read on the previous Runblogger post on stress fractures, I felt the need to do a little more research and so I did a Pub Med search and selected 22 articles to review which were based on the current literature regarding metatarsal stress fractures. I spent the better half of an entire long weekend reviewing the science behind ground reaction forces, force plate analysis, different footwear (racing flats vs. trainers), case studies claiming the incidence of stress fractures in newer minimalist footwear and the such. My conclusions: I am left with more questions than when I started.
Science is a challenging field. We are taught the scientific method from an early age. Formulate a hypothesis, test the hypothesis, and determine its validity. The literature is full of hypotheses, tested and untested. Ideas are examined and re-examined, papers written and revisited. It reminds me of the long standing argument over butter vs. margarine. Growing up we ate butter, then it was deemed unhealthy, so margarine became the new butter. Lo and behold we discovered trans fats, and suddenly we are back to butter. Suffice it to say, any argument or any hypothesis will be tested and retested and a counter argument can be made.
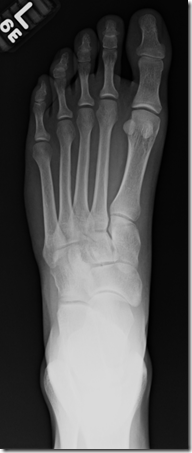
Keeping the above in mind, let’s get into the details. It is true that second metatarsal stress fractures are more common amongst runners, with third and fifth metatarsals occurring at a lower rate. Interestingly the stress fractures of the second metatarsal in runners tend to be distal as opposed to proximal which was described in ballet dancer (en pointe dancers specifically), suggesting that the latter is due more to compressive axial forces or axial and shearing forces as opposed to bending forces. I would agree with Dr. Kerrigan that the forces across the metatarsals are greatest at mid to late stance and it is the combination of these forces, along with muscle fatigue involving the intrinsic foot muscles, that eventually leads to stress fractures in the metatarsals. I have not come across any articles describing the frequency of stress fractures occurring on either the compressive (dorsal) or tension (plantar) aspect of the foot. When looking at stress fractures at other sites in the body there is a wide range of occurrence on both tension and compression sides of the bone. For instance, a common femoral neck stress fracture is seen in the calcar region, that is the inferior femoral neck or the compression side, although I have seen several cases on the tension side as well. Bones themselves tend to be stronger in compression (pushing together) than in tension (pulling apart), but it is unclear whether they will tend to fail in compression vs. tension when subjected to submaximal forces repeatedly. I would surmise that failure can occur on either aspect based on my experience. As for the metatarsal, I have seen both tension and non tension (medial and lateral) stress fracture lines.
As for bone remodeling in response to applied stress, it will occur according to Wolff’s law, that bone remodels according to the location of lines of stress. We see this at the femoral neck most apparently as one can radiographically visualize the curving lines of the trabeculae (little bony plates that make up the inner spongy bone) aligning to support the weight of the body. In one of the articles I read below, differences were seen between runners and soccer players, with soccer players having greater cross sectional diameter of the metatarsals. A suggested reason for this observation was that the bones were subjected to more forward, backward, and side to side motion as opposed to the continually straight ahead motion found in runners.
As for bone remodeling, this is a dynamic process dependent on the interplay between osteoblasts and osteoclasts (cells that respectively build and break down bone). From an imaging standpoint, osteoblastic response to injury can be seen as early as two weeks from onset of injury – with an MRI this can be seen as intramedullary edema (swelling inside the bony shaft, typically called a stress reaction) even before a stress fracture line is visible. It is important to note however that the laying down of new bone in response to stress is disorganized and that a delicate interplay exists between osteoblasts (bone building cells) and osteoclasts (bone removing cells) during the healing process. This interplay eventually allows for the most optimal healing to occur according to the load placed on the affected bone. This balance between osteoblast and osteoclast activity is disrupted with a stress fracture and repeated loading, thus the osteoclast wins out and the bone weakens thus leading to the fracture. Once this point is reached, the bone requires immobilization for optimal healing. All of the literature I’ve come across describes a rest period of approximately 6 to 8 weeks in adults, with shorter periods for children and adolescents. Also, all of the literature recommends a return to activity in a graded fashion to avoid re-injury. There is no description of a window at which point you would risk greater injury because that is variable amongst different individuals. For instance, my body is sore and my bones ache after a 9 mile long run this weekend, to the point that I know I risk injury by running the day after. Dean Karnazes goes out and runs 40 miles today and can do another 40 tomorrow. He’s just different, and so is his body.
There a multitude of suggested risk factors for the development of stress fractures. These include and are not limited to female sex, lower bone mineral density, smoking, malnutrition, poor training habits, being overweight or underweight (probably an aspect of nutrition), shoe wear (although the article that mentioned this as a risk factor did not articulate as to what type of shoe wear), and even a tight Achilles which may play a role in the angle of the metatarsals at push off, which can subject them to increased stresses. One interesting thing, and I have no way to prove it at this time, is that bone mineralization in consistently shod individuals will likely be less in the involved extremity than in the non-shod individual. I base this upon my experience in evaluating the x-rays of individuals who have been casted for any period of time or who have had surgery which resulted in non-weight bearing in an extremity. The trabecular bone density decreases dramatically in those injured or non weight bearing. Now a cast is an extreme example of a “shod” individual, but I firmly believe that the bones in the foot adapt over time to being chronically shod vs. unshod. When I get some good imaging examples I will be sure to share them as I am beginning to collect a series of images of running related injuries evaluated using radiologic technology.
There is certainly a great deal of information out there regarding these injuries. I am concerned that the recent study on stress fractures and Vibram Fivefingers footwear (Giuliani et al., 2011) stepped out so far as to suggest that it was due to the footwear since stress fractures have been around since the dawn of time and the research in runners from as far back as 1978 has shown the same frequency, and I can assure you Vibram was not around back then to take the blame. I am, however, also certain that stress fractures will occur in individuals wearing minimalist footwear and that they could be avoided by appropriately training so as not to disrupt the balance between osteoclast and osteoblast activity in the wrong direction.
Thanks for reading.
Andrew W. Lischuk, MD
Articles on Stress Fractures
1. Brockwell J, Yeung Y, Griffith JF. Stress fractures of the foot and ankle. Sports Med Arthrosc. 2009;17(3):149-59.
2. Carmont MR, Patrick JH, Cassar-Pullicino VN, Postans NJ, Hay SM. Sequential metatarsal fatigue fractures secondary to abnormal foot biomechanics. Mil Med. 2006;171(4):292-7.
3. Chuckpaiwong B, Cook C, Pietrobon R, Nunley JA. Second metatarsal stress fracture in sport: comparative risk factors between proximal and non-proximal locations. Br J Sports Med. 2007;41(8):510-4.
4. Drakonaki EE, Garbi A. Metatarsal stress fracture diagnosed with high-resolution sonography. J Ultrasound Med. 2010;29(3):473-6.
5. Edwards MR, Jack C, Jones GG, Singh SK. Post-operative stress fractures complicating surgery for painful forefoot conditions. Foot (Edinb). 2010;20(2-3):49-51.
6. Finestone A, Milgrom C, Wolf O, Petrov K, Evans R, Moran D. Epidemiology of metatarsal stress fractures versus tibial and femoral stress fractures during elite training. Foot Ankle Int. 2011;32(1):16-20.
7. Fredericson M, Jennings F, Beaulieu C, Matheson GO. Stress fractures in athletes. Top Magn Reson Imaging. 2006;17(5):309-25.
8. Gehrmann RM, Renard RL. Current concepts review: Stress fractures of the foot. Foot Ankle Int. 2006;27(9):750-7.
9. Giuliani J, Masini B, Alitz C, Owens BD. Barefoot-simulating Footwear Associated With Metatarsal Stress Injury in 2 Runners. Orthopedics. 2011;34(7):e320-3.
10. Goud A, Khurana B, Chiodo C, Weissman BN. Women’s Musculoskeletal Foot Conditions Exacerbated by Shoe Wear:An Imaging Perspective. Am J Orthop (Belle Mead NJ). 2011;40(4):183-91.
11. Gu YD, Ren XJ, Li JS, Lake MJ, Zhang QY, Zeng YJ. Computer simulation of stress distribution in the metatarsals at different inversion landing angles using the finite element method. Int Orthop. 2010;34(5):669-76.
12. Hetsroni I, Nyska M, Ben-Sira D, et al. Analysis of foot structure in athletes sustaining proximal fifth metatarsal stress fracture. Foot Ankle Int. 2010;31(3):203-11.
13. Laker SR, Saint-Phard D, Tyburski M, Van Dorsten B. Stress fractures in elite cross-country athletes. Orthopedics. 2007;30(4):313-5.
14. Logan K. Stress fractures in the adolescent athlete. Pediatr Ann. 2007;36(11):738-9, 42, 44-5.
15. Meardon SA, Edwards B, Ward E, Derrick TR. Effects of custom and semi-custom foot orthotics on second metatarsal bone strain during dynamic gait simulation. Foot Ankle Int. 2009;30(10):998-1004.
16. Niva MH, Sormaala MJ, Kiuru MJ, Haataja R, Ahovuo JA, Pihlajamaki HK. Bone stress injuries of the ankle and foot: an 86-month magnetic resonance imaging-based study of physically active young adults. Am J Sports Med. 2007;35(4):643-9.
17. Queen RM, Abbey AN, Chuckpaiwong B, Nunley JA. Plantar loading comparisons between women with a history of second metatarsal stress fractures and normal controls. Am J Sports Med. 2009;37(2):390-5.
18. Queen RM, Mall NA, Nunley JA, Chuckpaiwong B. Differences in plantar loading between flat and normal feet during different athletic tasks. Gait Posture. 2009;29(4):582-6.
19. Umans HR. Imaging sports medicine injuries of the foot and toes. Clin Sports Med. 2006;25(4):763-80.
20. Wall J, Feller JF. Imaging of stress fractures in runners. Clin Sports Med. 2006;25(4):781-802.
21. Wiegerinck JI, Boyd J, Yoder JC, Abbey AN, Nunley JA, Queen RM. Differences in plantar loading between training shoes and racing flats at a self-selected running speed. Gait Posture. 2009;29(3):514-9.
22. Zadpoor AA, Nikooyan AA. The relationship between lower-extremity stress fractures and the ground reaction force: a systematic review. Clin Biomech (Bristol, Avon). 2011;26(1):23-8.

















From your second paragraph:
“Andrew let me know that he’s most proud of being a devoted husband to MY wife Kim”.
Thems fightin’ words! I’m sure you meant “his” wife Kim. ;)
Stupid grammar. Thanks for the tip!
Would be nice if they could test for their vitamin D to see if there is a correlation. My hunch is on vitamin D deficiency for slowing down or interfering proper bone modeling.
http://www.prnewswire.com/news…
Ironically, liberal usage of sunblock significantly raises risk of getting one of 18 different cancers (maybe more) including skin cancer melanoma. Like Andrew pointed out butter-margarine problem, It’s like that with sunblock lotion… Consistent sun exposure without sunblock lotion but no sunburn keeping vitamin D in the optimal range actually prevent melanoma but inconsistent sun exposure somewhat increases risk of getting melanoma due to lower vitamin D level. Dermatologists tend not to be not very well versed in vitamin D research unfortunately but they are slowing catching up if at all. Lots of new scientific research coming out on vitamin D in many areas. We’re finally catching up. 600IU that is currently recommended is far too low. The general rule of thumb should be 1000 IU for every 25 lbs of body weight for healthy people which would keep vitamin D level within 50-80 ng/ml range. This is extremely important during cold months as it significantly cut down risk of getting cold, flu, and other upper respiratory illnesses.
Amazing lit review Andrew on an area most of us do think of in this detail.
Can you bring an ultrasound bone densitometer to the NYC Barefoot Run in September. With some prescreening of the true barefooters and their volume we may have a good sample to compare against controls. Pete you’re in…right? Give away some beer as the study incentive and you’ll have lots of players. Hard to get a large sample of western barefoot runners as opposed to barefoot livers (developing country) and this may be the ticket.
I think you will discover lots of interesting things in foot thickness, muscle, and bone strength.
Mark Cucuzzella
A bone densitometer study would be very interesting, and you’re right on about the sample opportunity. Hmm….
Thanks Mark, I like your idea about the densitometry study, but we don’t use us density measures at Yale, still using dexa. One of our foot arthropods is doing a lot with us imaging to evaluate the foot tendons though. I guess we can petition hologic to give us a loaner though! I wonder how you would put the free beer in the research proposal, might irk the folks on the IRB.
So I’ll ask a question on my own blog comment section. Is it possible to tell the difference between a stress reaction and the normal remodeling response? I think the remodeling issue is really critical to this whole issue, and bone is likely to get weaker for a period after exposing it to a new stress before it gets stronger.
I’ll refer you to this study:
Skeletal Radiol. 2001 Feb;30(2):61-6.MRI abnormalities of foot and ankle in asymptomatic, physically active individuals.Lohman M, Kivisaari A, Vehmas T, Kallio P, Malmivaara A, Kivisaari L.They looked at 19 marathon runners post race with MRI and found areas of signal abnormality that are usually referred to as stress response and yet the athletes were asymptomatic. This leads to the conclusion that MRI findings do not always match clinical symptoms. The answer still lies out there somewhere.As an aside, I saw at least 3 brave souls (or soles) on my trail run today (some areas of gravel) running barefoot. I am not as brave and have resurrected my Kinvaras for now as my adidas adizero I feel are too narrow for my forefoot, despite my narrow width foot as it is. There were giving me metatarsal pain which I found humorous since it was the subject of this topic.
I am just getting over a stress fracture but it was in my toe, not my metatarsal. A lot less common, but do most of the same physiological forces apply to the cause?
If it was a true stress fracture, I’d say yes. Stress fractures are overuse injuries where the bone is stressed faster than it can repair.
Back in the spring, I went to the podiatrist because of pain in 5th metatarsal. X-rays showed I had broken 2nd and 3rd metatarsal (explains TOFP a few weeks before visit, I guess) and they had healed up but not perfectly. The Dr. said the pain in the 5th was due to pressure caused by the weakness now in the 2nd & 3rd and, of course, recommended custom orthotics. I did not get them. To me the Dr. implied my 2nd and 3rd would always be weak, even saying this weakness increased the likelihood of breaking the 5th. Is this researching saying this is not necessarily the case?
Bones will heal and with time will return to their original strength and appearance unless markedly deformed to begin with or something else interfered with healing. If you consciously or subconsciously changed your gait due to the 2nd or 3rd metatarsal fractures you could have subjected your 5th to altered/abnormal stresses which can lead to fracture. I can’t comment on orthotics since I am not as experienced or educated in that regard. My personal opinion is to avoid them but some of that is personal bias which led me to a site like this one in the first place. I think another good site to check out for sound research backed running med advice is the speed lab site at the university of Virginia, lots of really exciting work is being done their using some of the latest technology and slo motion video. If I continue to have my own issues with posterior tibial tendinitis I think I may head down there for an analysis.
Great post, keep them coming!
Unexpected things might just happened anywhere and anytime. That is why safety and proper knowledge about different things might be a big help.
Thank you for sharing this article with us.
Not sure I agree that unshod runners will have stronger metatarsal bones than shod runners. I think your analogy to casting is flawed–when one foot or leg is in a cast, it bears little or no weight, and hence bone mineralization is reduced (weight-bearing activity being the main driver of increased bone density). But in running, for a given runner at a given pace, the absolute weight supported by the bones is the same regardless of the footwear or lackthereof. Different shoes (or no shoes) CHANGE where stress goes, and can change the loading rate of the impact (the unshod condition actually increasing the loading rate), but can’t change the absolute amount of force going through the feet, especially if we accept Dr. Kerrigan’s hypothesis that forces and the risk of injury are greatest at midstance–in that case, footstrike style would have VERY LITTLE to do with injury risk, as the force at midstance is similar regardless of footstrike patterns (but are the internal forces the same? A forefoot striker should have more energy rebounding from the stretch-shortening cycle of the Achilles/calf).
I do think that shod runners will have different PATTERNS of bone mineralization, because the way they stress their metatarsals is different than how an unshod runner (especially a forefoot striker) would stress them. Abruptly changing the stresses on the foot (by switching to barefoot running, for example) would stress the bone in a way it is not used to, causing a stress fracture. Of course under this philosophy, an unshod runner would be at a similar risk if jumping into wearing shoes!
On a completely unrelated note, I’d be interested to know if Morton’s toe (having a longer second toe than big toe) is at all a factor in making second metatarsal stress fractures more common than 3rd, 4th, or 5th. A runner with morton’s toe would have the second metatarsal head on the ground slightly longer (since the metatarsal is longer) than any of the other metatarsal heads, and that might cause more force to be directed into that metatarsal vs. the other four. Thoughts?
I agree with most of what you are saying here – absolute force will be the same, but how and where specifically it is applied will change. One of the big differences when barefoot is that it’s quite possible that force under the second met head will be magnified since there is no shoe sole underneath to spread force application out. If you have force application focused on a smaller area, stress in this area will increase, and thus bending of the second met could increase as a result.
I do suspect Morton’s toe might raise the risk for the reasons that you suggest.
John,
You make a great point regarding the distribution of forces in the foot in the shod vs. unshod state and I agree with your comments above. I agree that the pattern of distribution of those forces change in one state vs. the other. My use of the cast analogy was an extreme example to show demineralization, as I have seen several stress fractures occur in patients who are coming back from injuries who have been recently casted. I do however, believe that shoewear may have some impact on bone density, I just don’t have the scientific backing to prove it. That impact may be like you said, in the pattern of distribution. For instance, traditional bulky shoes are less flexible which would distribute the forces along the foot differently so your bones will adapt to those forces and if you change to minimalist/more flexible, shoewear the force distribution will be different. It becomes quite complicated when you think about it, and designing a study to determine this with current technology would be frought with uncontrolled variable. None the less, your thoughts are well recieved.
As for the Morton’s toe, I agree with Pete’s reply. The length of the second toe will see increased forces on that metatarsal during the midstance phase over a longer duration of time. It would thus be logical to expect more injuries with these runners.
I have been thinking recently about the instances of fractures in the 2nd and 3rd metatarsals and it occurred to me that the perhaps lack in strength in the big toes and muscles, fascia and ligaments supporting the 1st metatarsal might have role to play in these injuries. If the 1st matatarsal isn’t doing it fair share I could see the 2nd and 3rd metatarsals being overused.
In particular I wonder about the way that big toe is bent inwards by years of poorly designed and fitting shoes, if the big toes isn’t in good alignment with the 1st metatarsal then the amount of force we can apply through the big toe and the 1st metatarsal.
I recall a post of Mark Cucuzella about use of Correct Toes spaces, and the importance of the alignment of the big toe for running barefoot. This made sense to me at the time, but I didn’t then ponder on the role of distribution of load across the toes and metatarsals.
Is this plausible? Could we get feedback from those with 2nd and 3rd metatarsal injuries as to whether their big toes is well aligned to their 1st metatarsal or not. Any X-rays taken of the feet would be ideal for doing such a review.
If this little theory does have some merit then Correct Toes or similar tool for bringing the toes back into alignment might well be a good way to develop foot structure that is better able to deliver the loads we demand of them. If one had a metarsal injury already perhaps looking at solving this part of the problem will help, or if new runners (or new to barefoot/minimalist) would be to look at solving the big toes alignment prior to introducing too much barefoot/minimalist running.
As a wee note, my own big toes still are not perfectly aligned despite being barefoot for most of the last year. Sitting at desk barefoot probably doesn’t count too much though!
Robert,
Funny you write this at this time – we’ve just been having this same discussion on a forum that I’m a part of. Here’s what I wrote on the issue:
This was kind of the post that I never got to when I was attempting to track down the cause of met stress fractures. Quite simply, I think the toes, particularly the big toe, play a big role in reducing bending stress to the mets. I notice that I get 2nd met head ache only when I run in certain types of Fivefingers if the tightness of the fit on the toes prevents me from effectively flexing them. It seems that a large number of the 2nd met stress fractures among people trying minimalism occur in people wearing Vibrams, so there could be a design element in toed shoes that limit toe flexion that is a culprit.
2nd met fractures are not uncommon in traditionally shod runners, but a thicker sole tends to reduce focal stress under the mets by spreading it out a bit over a wider area, and you lose this when you go barefoot or wear a very minimal shoe. So, shoes mess up our toes, and they don’t allow us to adapt to more focal stress under the met heads. Take your shoes off suddenly and you get a double whammy – weak mets and poor ability of the toes, particularly the big toe to compensate by flexing to offload force. So, I think a lot of met stress fractures are the result of negative shoe adaptations that are manifested when shoes are taken away. I should note
that big toe flexors have been shown to increase in strength through
training in flexible shoes (Nike Frees).
I think you would enjoy this paper – it essentially describes this very
phenomenon as it relates to stress fractures and points out how this can be
exacerbated by hallux valgus:
http://www.ncbi.nlm.nih.gov/pm……<http: url?sa=”D&q=http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1233023/pdf/janat00239-0128.pdf&usg=AFQjCNHO6gOa-u62YmdaKcrXPyUq63uhKQ” http://www.google.com=“”>
Pete</http:>
How soon would a stress fracture/reaction show up on plain X-ray? I have been transitioning my running for 16 months without problems and have been progressively increasing my mileage for marathon prep. After 18 miles yesterday I have pain over my 3rd metatarsal and am VERY worried. I only have 6 weeks to my event. It could be just a strain as I was on some very broken up asphalt at times, but 3rd met is tender to palpation. Do I race to the doctor for any diagnostics now and if so what should I push for?
Wish I could help you, but I’m not a medical doc – rest it for a bit and if it doesn’t improve, always best to see a pro and get it sorted out.
—-
Pete Larson’s Web Links:
My book: Tread Lightly – http://ow.ly/bdUO0
Blog: https://runblogger.com
Twitter: http://twitter.com/oblinkin
Facebook: https://www.facebook.com/Runbl…
Thanks, I appreciate that, I thought maybe Dr. Lischuk might have some thoughts on it.
Cheryl,
Sorry about the delay. I had written a response earlier but it seems it did not post. Pete actually wrote me an email asking about your question today so I am reposting my response below and want to 1. thank you for your question and 2. thank Pete for taking the time to look out for you in reminding me that my original post did not register. So here goes:
The bottom line is that it may take up to two weeks to actually visualize a stress fracture on a plain radiograph if the stress fracture is big enough to see. we basically look for periosteal reaction which is the body’s way of healing the stress fracture, sometimes all we see is some cortical thickening in the area, again as the bodies response to lay down more bone in the area undergoing the abnormal stresses. MRI is very sensitive to evaluate for stress reaction and stress fractures even in the early stages but the cost and time needed to get a scan may be prohibitive and some insurance will not cover it for the sole indication of stress fracture evaluation. The bottom line is that if this is concerning enough, then the best bet is to be evaluated by a physician knowledgable in this field, either a podiatrist or orthopedic surgeon since the internet prohibits me from really doing a good physical exam and history which remains the mainstay of any good medical therapy. I wish you the best of luck and hope you are able to compete in her race. Above all, be careful and listen to your body. There are many races to run.
Sincerely,
Andrew W. Lischuk
Thank you for taking the time to respond so in depth. I had suspicion that diagnostics would not be helpful so early in the process. Thanks for confirming this and helping me to remain patient.